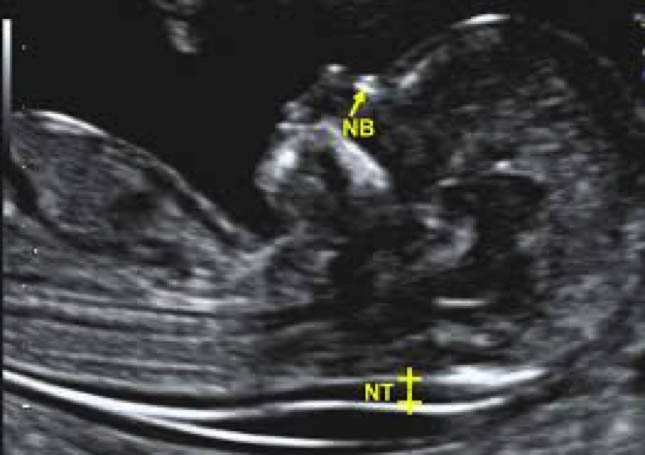
Nuchal Scan
This scan is carried out from 11 weeks to 13 weeks and six days. The scan is usually performed transabdominally but in a few cases it may be necessary to do the examination transvaginally.
Aims of the nuchal scan
To date the pregnancy accurately
This is particularly relevant for women who cannot recall the date of their last period, have an irregular menstrual cycle, or who have conceived whilst breastfeeding or soon after stopping the pill. We measure the size of the fetus and from this we calculate the expected date of delivery.
To diagnose multiple pregnancy
Approximately 2% of natural conceptions and 10% of assisted conceptions result in multiple pregnancy. Ultrasound scanning can determine if both babies are developing normally and if the babies share the same placenta which can lead to problems in the pregnancy. In such cases it would be advisable to monitor the pregnancy more closely.
To diagnose fetal abnormalities
Some major abnormalities may be visible at this gestation. However it will still be necessary to have a 20 week morphology scan.
To assess the risks of chromosomal abnormalities such as Trisomy 21 (Down’s Syndrome)
Each woman will be given an estimate of her individual risk for this pregnancy. This is calculated by taking into account the:
- Age of the mother
- Measurement of two hormones in the mother’s blood – PAPP-A (Pregnancy associated plasma protein-A) and BhCG (Beta human chorionic gonadotrophin)
- Ultrasound scan findings of nuchal translucency thickness, nasal bone, blood flow through the fetal heart and ductus venosus and fetal abnormalities.
Parents will receive full counselling concerning the significance of these risks and the various options for further investigations if indicated, including Non invasive Prenatal Testing (NIPT) or invasive testing (CVS or Amniocentesis).
Your referring doctor will provide you with a request form for a blood test. We recommend you have the bloods taken 4-5 days prior to you ultrasound scan, so the results are available to our clinicians in order to provide you with your complete First Trimester Risk Assessment on the day of your scan.
It is useful to have a moderately full bladder, which can allow a better picture of the baby as your bladder pushes the uterus up above the pelvic bone. An hour before your appointment, please empty your bladder and drink 2 standard glasses of water. Please do not go to the toilet again until after your scan. We do not need you to have an uncomfortably full bladder. Please talk to our reception staff if you are uncomfortable while waiting for your scan.
You are welcome to have members of your family join you for the scan. It is important to remember that this is a diagnostic procedure and the sonographer will need to concentrate on the images of your baby.
About Us
The Canberra Fetal Assessment Centre (CFAC) is a complete and unique obstetrics and gynaecology ultrasound service. Our experienced doctors and sonographers provide an expert service specialising in maternal and fetal Medicine and women’s health.
Address
- CFAC Bruce
85/15 Braybrooke Street
Bruce ACT 2617
- CFAC Deakin
Suite 3-7,
175 Strickland Crescent
Deakin ACT 2600
Phone
(02) 6162 0582
hello@cfac.com.au